what age and how many eggs made it to blast
Higher Success Rates Per Transfer
A crucial concept to get down is that embryos that are grown to the blastocyst phase are far more likely to lead to a alive nascency than embryos that have arrived only at the cleavage phase. Below is an analysis of over ane,600 patients across fifteen studies that demonstrates that transfers that use blastocysts are nearly i.5x more than likely to lead a live nascency than transfers that utilise cleavage-stage embryos. The net effect is that patients suffer fewer failed transfers when they have blastocysts transferred than when they take cleavage phase embryos transferred.

Safer Unmarried Embryo Transfer
An boosted benefit of having more confidence in an embryo's potential is that doctors and patients are much more than prepared to transfer one embryo at a fourth dimension. Below you can see data on all constituent single embryo transfers in the United States from 1999 - 2010: nearly lxxx% were washed using embryos grown to the blastocyst stage. But how reluctant were doctors to do a single embryo transfer with cleavage phase embryos? Less than 0.6% of transfers relying upon cleavage stage embryos occurred using only 1 embryo.

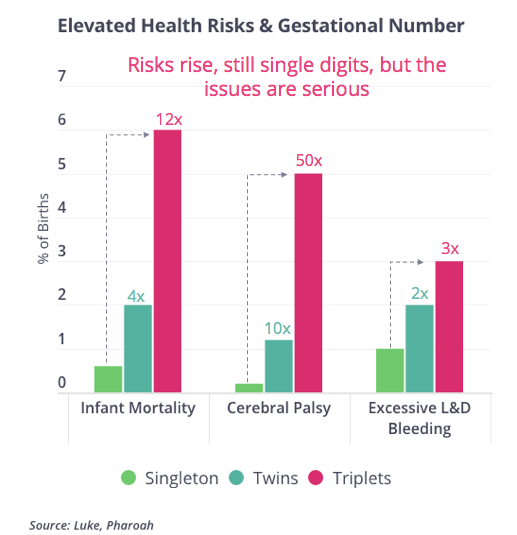
The likelihood of twins and triplets drops significantly when embryos are transferred one at a time. As yous can run across below, twin and triplet pregnancies present a threat to both the female parent and offspring. Thus, some would argue using blastocyst stage embryos is safer because it helps united states avert the temptation of risky transfer behavior that could endanger mother and offspring.
Safer For Genetic Testing
Next, growing embryos to blastocyst helps if someone wants to have embryos genetically tested before transfer. Every bit you'll encounter in the next lesson, when testing predicts that an embryo has the wrong number of chromosomes, it nearly never results in a live birth. Equally a result, genetic testing can help cut down on transfers that don't implant or end in miscarriage. Just it costs $3,000 - $5,000 and does not exercise anything to change the underlying quality of a patient's embryos, pregnant it doesn't change the odds that an egg retrieval cycle volition work. Thus, many debate the value of genetic testing of the embryos.
Genetic screening requires a fertility dispensary to cut off a few cells from the embryo to test. As you can run across from a well-regarded (but even so small, unmarried center) written report beneath, taking a few cells from a cleavage phase embryo does more than harm than taking cells from a blastocyst phase embryo. The touch on shows upwards in the form of lower implantation rates (and presumably lower nativity rates). Thus, if y'all want to exercise genetic testing, it's far safer to grow embryos to the blastocyst phase. In fact, if your clinic does genetic testing on cleavage stage embryos, that'southward a red flag.

In many ways, growing an embryo to the blastocyst stage and then genetically testing it applies two option filters on which embryo to utilize. Should the transfer fail (remember, most practise), having characterized the embryo equally strong enough to reach blastocyst stage and as being "chromosomally-normal" may exist a outset indicator that more work needs to be done to assess the uterus. However, it doesn't necessarily mean the uterus represents a challenge since even PGT-normal blastocyst transfers still simply piece of work ~threescore% of the time (as y'all can see below). Nevertheless, after 3 successive transfers with PGT-A normal embryos alive nativity rates tend to hover around 90% and and so at this point, clinicians may rightly get-go to suspect the uterus equally representing a challenge.
If whatsoever embryos is grown just to cleavage phase, it's unclear if it was stiff enough to reach the blastocyst stage and we weren't given the run a risk to know if it was chromosomally normal. As a outcome, it can be harder to make up one's mind whether the crusade of a failed transfer was due to poor embryo quality or another issue with implantation.
Safer Freeze and Thaw Cycles
Finally, growing embryos to the blastocyst phase can be a skilful thought if the patient wants to freeze embryos and transfer them later. Every bit we'll evidence in a future lesson, freezing embryos and delaying a transfer allows a woman's hormonal balance to restabilize and for the transfer to happen when her uterus is virtually receptive.
Many doctors believe the freeze-thaw process is more likely to go well with blastocysts rather than cleavage phase embryos. Below are the better run studies (the names in each blue box represent the written report'south author) characterizing how often embryos are frozen and then thawed intact. As you lot can see on the right, over 90% of embryos that are frozen can exist thawed intact. For cleavage stage embryos that number is in the loftier 70s to mid 80s. In practical terms, compared with blastocysts, this means 1 additional cleavage phase embryo will go lost for every ten frozen. In our minds that is a moderate difference and in the 1000 scheme of things is one of the slightly less compelling reasons to favor blastocysts over cleavage stage embryos.

andersonkillaimpon.blogspot.com
Source: https://www.fertilityiq.com/ivf-in-vitro-fertilization/cleavage-vs-blastocyst-embryos-day3-day5
0 Response to "what age and how many eggs made it to blast"
Publicar un comentario